Managing Acid Reflux
Local-Friendly Lifestyle Tips and Treatment Options for GERD
Acid reflux is one of the most common conditions I treat in the office. Many patients describe a burning sensation in the chest after meals, regurgitation of sour liquid, chronic throat clearing, or even a persistent cough. When these symptoms occur regularly, we call it Gastroesophageal Reflux Disease (GERD), Heartburn, or Reflux.
GERD develops when stomach acid repeatedly flows backward into the esophagus. Over time, this can irritate the lining of the esophagus and significantly affect quality of life. The good news is that most cases can be managed very effectively with lifestyle adjustments and, when necessary, medication.
What Is GERD?
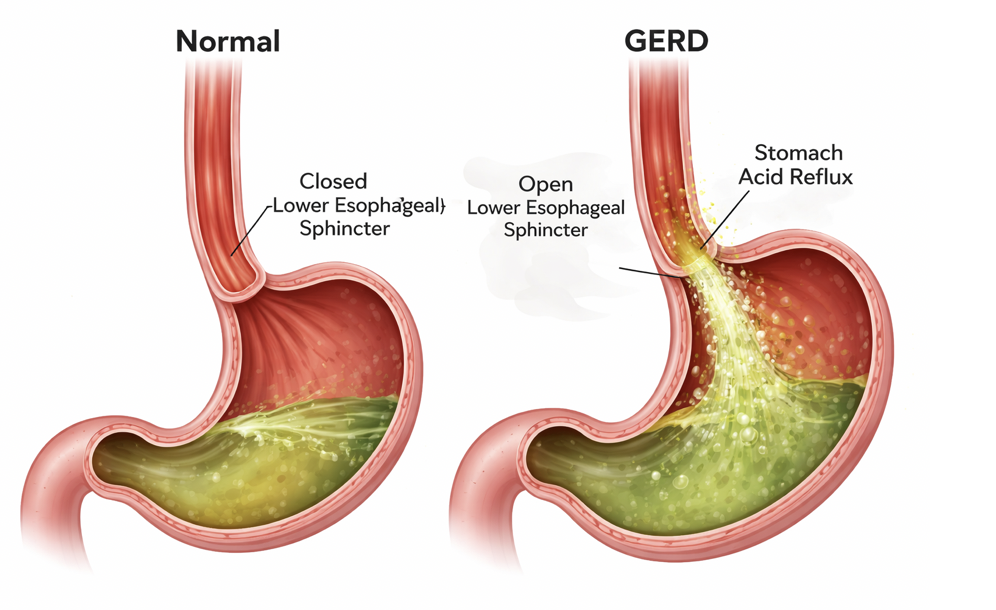
GERD occurs when the lower esophageal sphincter (LES) — a muscular valve between the esophagus and stomach — relaxes or weakens at inappropriate times. This allows acid to travel upward.
Common symptoms include:
Heartburn (burning in the chest)
Regurgitation
Difficulty swallowing
Chronic cough or throat irritation
Hoarseness
Worsening symptoms when lying down
If left untreated, GERD can lead to complications such as esophagitis, strictures, or a condition called Barrett's esophagus, which can increase the risk of esophageal cancer.
Local-Friendly Lifestyle Tips to Reduce Reflux
Many patients are surprised how much improvement they can achieve with targeted lifestyle changes. Here are practical strategies that fit into everyday life:
1. Adjust Meal Timing
Avoid eating within 3 hours of bedtime.
Consider your local dining habits — late dinners are common in many communities. If dinner must be late, keep it lighter.
2. Modify Common Trigger Foods
Typical triggers include:
Fried or greasy foods
Tomato-based dishes
Spicy meals
Chocolate
Mint
Coffee
Alcohol
Rather than eliminating everything at once, identify your personal triggers. A simple food diary for two weeks can be very helpful.
3. Elevate the Head of the Bed
For nighttime symptoms:
Raise the head of your bed 6–8 inches using risers.
Extra pillows alone are usually not effective.
4. Maintain a Healthy Weight
Even modest weight loss can significantly reduce reflux symptoms by decreasing abdominal pressure.
5. Avoid Tight Clothing
Tight belts or waistbands can increase pressure on the stomach and worsen reflux.
6. Quit Smoking!
There are so many reasons stop smoking, but specifically with GERD smoking weakens the lower esophageal sphincter and increases acid exposure.
Medical Treatment Options
When lifestyle adjustments are not enough, medications can be very effective.
1. Antacids (Over-The-Counter)
Examples include:
Tums
Mylanta
These work quickly but are short-acting.
2. H2 Blockers (Over-The-Counter)
Examples:
Famotidine (Pepcid)
They reduce acid production and can be helpful for mild to moderate symptoms.
3. Proton Pump Inhibitors (PPIs)
Examples:
Omeprazole
Pantoprazole
These are the most effective medications for healing inflammation and controlling frequent symptoms. They are typically taken once daily before breakfast. These can be Over-The-Counter at lower doses and for short term use (up to 2 weeks). Beyond that they should involve a doctor and a prescription.
Many patients worry about long-term safety with PPIs. For appropriate patients, PPIs are very safe and often necessary. However, they should be used at the lowest effective dose and periodically reassessed with your physician.
4. Potassium-Competitive Acid Blockers (PCABs)
A newer class of acid-reducing medication is called Potassium-Competitive Acid Blockers (PCABs).
One example is:
Vonoprazan (brand name Voquezna)
PCABs work differently from traditional Proton Pump Inhibitors (PPIs). While PPIs need to be activated in the stomach and may take several days to reach full effect, PCABs:
Work more quickly
Provide stronger and more consistent acid suppression
Do not need to be timed as strictly before meals
For some patients — particularly those who continue to have symptoms despite PPI therapy — PCABs may be an effective alternative.
Like all medications, they are not necessary for everyone. Treatment choice depends on symptom severity, response to prior therapy, and individual medical history.
When Should You See a Gastroenterologist?
Seek evaluation if you experience:
Difficulty swallowing
Unintentional weight loss
Persistent vomiting
Black or bloody stools
Symptoms that do not improve with treatment
In these cases, an upper endoscopy may be recommended to evaluate the esophagus and stomach.
A Balanced Approach
GERD is very common, and in most cases, it is very manageable. The key is an individualized plan that combines:
Practical lifestyle adjustments
Smart use of medication
Appropriate monitoring
If you are experiencing persistent reflux symptoms, don’t ignore them. Early management prevents complications and improves daily comfort.
As with many gastrointestinal conditions, small changes can make a significant difference.